Neuroinflammation
Neuroinflammation is a host-defense mechanism in the CNS, which protects normal brain function and structure in response to injury and infection. This may be beneficial by leading to the clearance of unwanted material and dying cells in healthy brain development, but also pathogenic in the induction of neuronal cell death and production of antibodies against CNS proteins.
Neuroinflammation Product Areas
The CNS is immune privileged, in that the blood brain barrier (BBB) protects it against peripheral circulating antibodies and the infiltration of peripheral immune cells. Immune response and inflammation in the CNS are regulated by microglial cells and their communication with other cell types, with the resulting processes being helpful and/or harmful.
Microglia are the key effector cells of neuroinflammation and are constantly surveying the cerebral environment to detect even the smallest pathogenic change. These cells belong to the myeloid cell lineage and enter the CNS during early embryonic development, with physiological roles in CNS development and mature synapse pruning. Microglia act as 'scavengers' in the CNS, removing damaged/apoptotic cells and protein plaques and tangles, through phagocytosis mediated by the complement system. Additionally, microglia communicate with and influence other CNS cells including astrocytes and neurons, releasing chemokines as well pro- and anti-inflammatory cytokines. The release of anti-inflammatory cytokines, as well as their ability to recruit neurons and astrocytes to sites of tissue damage allow microglia to promote tissue repair following neuroinflammation. However, microglia can also cause neurodegeneration through the production of proinflammatory cytokines and other cytotoxic substances to induce neuronal cell death.
There are no resident antigen presenting cells within the CNS, however when activated in response to tissue damage or injury, microglia can act as antigen presenting cells. When the BBB is compromised, peripheral circulating T-cells can cross the BBB and become activated by microglia that are presenting antigens. The production of antibodies against CNS proteins by infiltrating peripheral immune cells leads to autoimmune neurological disorders such as myasthenia gravis (MG). Inflammation resulting from damage to the BBB and infiltration of peripheral T-cells is also a pathogenic feature of multiple sclerosis (MS) and causes demyelination.
Neuroinflammation and immune response have been identified in neurodegenerative disorders, where they are a key pathogenic feature leading to cell death in Alzheimer's disease, amylotrophic lateral sclerosis, Parkinson's disease and MS or the primary cause of disease as in MG. Additionally neuroinflammation has also been identified as a feature of multiple neurological disorders such as depression and schizophrenia.
Literature for Neuroinflammation
Tocris offers the following scientific literature for Neuroinflammation to showcase our products. We invite you to request* or download your copy today!
*Please note that Tocris will only send literature to established scientific business / institute addresses.
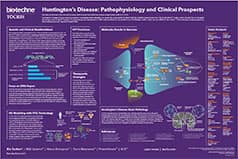
Huntington's Disease Poster
Huntington's disease (HD) is a severe monogenic neurodegenerative disorder, which is characterized by the prevalent loss of GABAergic medium spiny neurons (MSN) in the striatum. This poster summarizes the effects of mutant huntingtin aggregation implicated in the pathology of HD, as well as highlighting the use of iPSCs for HD modeling.
Parkinson's Disease Poster
Parkinson's disease (PD) causes chronic disability and is the second most common neurodegenerative condition. This poster outlines the neurobiology of the disease, as well as highlighting current therapeutic treatments for symptomatic PD, and emerging therapeutic strategies to delay PD onset and progression.